Japan Agency for Medical Research and Development, Research Program on HIV/AIDS
The study group on "A study on the management of opportunistic infections associated with early and prolonged use of ART"
Principal investigator: Katsuji Teruya
Questionnaire results
Trends in the Incidences of Non-AIDS–defining Malignancies in Patients Infected with Human Immunodeficiency Virus
| Investigators: | Koichi Izumikawa (Department of Infectious Diseases, Unit of Molecular Microbiology and Immunology, Nagasaki University Graduate School of Biomedical Sciences) |
| Research coordinator: | Takeshi Tanaka (Nagasaki University Hospital Infection Control and Education Center) |
Abstract
To elucidate the current status of non-AIDS–defining malignancies in patients infected with human immunodeficiency virus (HIV), a questionnaire survey was conducted across 378 core HIV hospitals. Responses were received from 117 hospitals (response rate, 31.1%). In 2023, 78 patients were diagnosed with malignancies. This number was almost comparable to that diagnosed in 2022 (76 patients). Based on the cumulative incidence of malignancies, the most common malignancy was lung cancer, followed in descending order by colorectal, gastric, and liver cancers; anal, other hematologic, head and neck, and other urological tumors; and laryngeal cancer. Although the distribution of cluster of differentiation (CD)4 cell counts at the onset of malignancies showed that more patients had lower CD4 cell counts, the distribution gradient of the counts was small; even some patients with high CD4 cell counts developed malignancies. These distributions greatly differed from the distribution of CD4 cell counts at the time of diagnosis of opportunistic complications. The most common age at onset of malignancies was 60–69 years. Of the patients, 81.9% developed malignancies 1 year or more after being diagnosed with HIV infection. The posttreatment complete and or partial remission rate was 63.1%. The findings of this study suggest that long-term follow-up of patients with HIV should include regular monitoring for the development of malignancies as well as patient education on smoking cessation with respect to the risk of lung cancer. Furthermore, the noticeable increase in the incidence of colorectal cancer over time indicates a need for screening for colorectal cancer.
A.Objective
Health management over the long term has been recognized as an important issue in the treatment of human immunodeficiency virus (HIV) infection. This recognition is based on accumulated data involving the early initiation of antiretroviral therapy and daily management procedures. The development of malignancies is regarded as part of this issue. Opportunistic infection study group, funded by the Health, Labour and Welfare Sciences Research Grant of the Japanese Ministry of Health, Labour and Welfare, has also monitored the trend in the development of non-AIDS–defining malignancies from when the reported incidences of malignancies were high in patients with HIV. This study group reported that the incidences of non-AIDS–defining malignancies are relatively high in patients with HIV, and that the incidences recorded for these patients differ from the corresponding incidences in the general population in Japan. These findings have prompted studies on malignancies, including leukemia. We conducted the 2024 study to investigate the non-AIDS–defining malignancies that occurred in 2023, in addition to the trend in the development of opportunistic infections complicating HIV infection, The data on the development of malignancies accumulated in the present study represent the only source for examining the nationwide trend in malignancy development among patients with HIV in Japan.
B.Methods
HIV infection is preferentially treated at core HIV/AIDS hospitals in Japan. Therefore, the present study was conducted by sending questionnaires to these hospitals and requesting their completion. The questionnaire for the present study on malignancies (![]() Appendix 2) was enclosed with the questionnaire used for the epidemiological study on HIV-associated opportunistic complications and sent to core HIV hospitals with a request for responses. Because previous studies accumulated data on malignancies that occurred between 1995 and 2006, our study group has collected longitudinal data since 2007. For the present study, we added data on malignancies diagnosed in 2023 to this dataset.
Appendix 2) was enclosed with the questionnaire used for the epidemiological study on HIV-associated opportunistic complications and sent to core HIV hospitals with a request for responses. Because previous studies accumulated data on malignancies that occurred between 1995 and 2006, our study group has collected longitudinal data since 2007. For the present study, we added data on malignancies diagnosed in 2023 to this dataset.
In the present study, we primarily aimed to elucidate the current status of the development of malignancies through gaining the cooperation of as many hospitals as possible. The questionnaire items were designed to be simple and were limited to the minimum number of items necessary. To improve the response rate for the questionnaire survey, the questionnaire items were limited to those that could be answered without a detailed review of the medical records of each patient. Consequently, elucidating the detailed status of each type of malignancy was difficult. This lack of detail is a limitation of the present study. To determine an accurate response rate, we enclosed return sheets with the questionnaires and requested that hospitals with no relevant cases reported the lack of data by using these sheets. The data collected were entered and compiled into a database using Microsoft Access. To exclude duplicate cases reported by the same hospital across years and duplicate cases reported by referring and referred hospitals, cases with identical data on birth year, disease name, year of onset, region of reporting hospital, and so forth were regarded as duplicate cases and unified. Cases of non-Hodgkin’s lymphoma, brain lymphoma, cervical cancer, and Kaposi’s sarcoma, which are AIDS-defining malignancies, were excluded from the aggregated data. To compare the prevalence between patients with HIV and the general population in Japan, the collected data were compared with the latest cancer statistics data in Japan (2014) available on the website of the Center for Cancer Control and Information Services at the National Cancer Center of Japan This study was reviewed and approved by the Ethics Committee of Nagasaki University Graduate School of Biomedical Sciences, as required by the Ethical Guidelines for Medical and Biological Research Involving Human Subjects, as partially revised on December 22, 2017. We designed the questionnaire survey to meet the requirements for data provision in response to requests from various institutions, as specified in the ethical guidelines for epidemiological studies. For example, to prevent the data analysis center from collecting the personal information of patients, we did not include questions asking for any personal information in the questionnaire; we also instructed the hospitals not to provide any personal information, including patient identification, on the questionnaire. Although the data collected were anonymized, they were handled with due care and analyzed in a controlled laboratory environment in which only the study investigators had access to them because they contained information on patients with HIV.
C.Results
In 2023, 78 cases of malignancy were reported. According to the annual number of reported cases (Figure 1), the incidence of non-AIDS–defining malignancies substantially increased to 9 cases in 2000 and further increased each year thereafter. Although it fluctuated in the subsequent years, since 2010, the incidence has leveled off at approximately 40–50 cases. The highest incidence was recorded in 2017. Although the incidence slightly decreased again in 2018, it has fluctuated at ~70 cases since then.
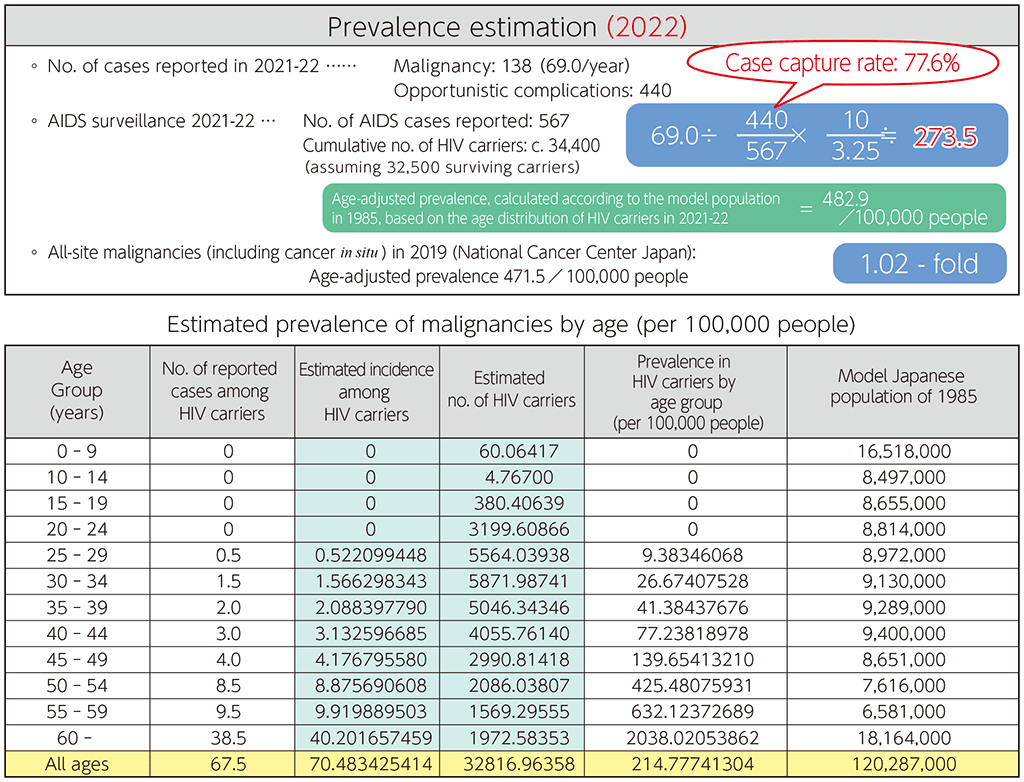
Owing to the substantial influence of year-to-year fluctuations, we calculated the mean incidence of malignancies per year and the prevalence per 100,000 people from data covering a 2-year period from 2022 to 2023. The present study comprised a questionnaire survey; consequently, the estimated capture rate was calculated by simultaneously comparing the number of cases of opportunistic infection reported in the survey conducted with the number of cases of AIDS reported by the AIDS Surveillance Committee (79.0%). Based on the assumption that the current number of surviving patients with HIV was approximately 33,400 people, the prevalence per 100,000 people was calculated as 297.0. The age-adjusted prevalence calculated based on the model population in 1985 was 438.4 per 100,000 people. This is 1.24 times higher than the prevalence of cancer (including carcinoma in situ) of 471.5 among the Japanese in 2014 (1.02 times, based on the 2021–2022 survey).
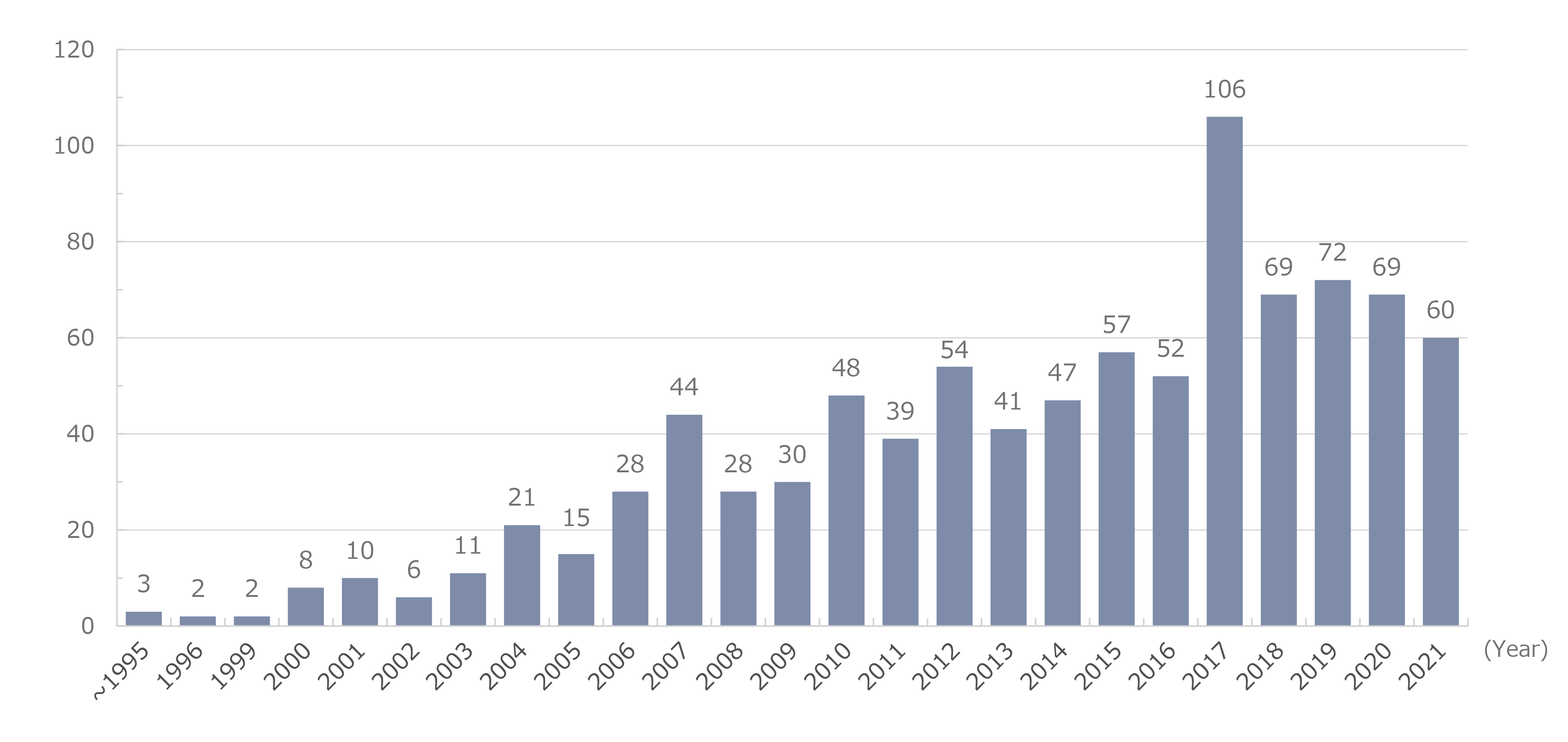
Figure 1. Annual number of cases of non-AIDS-defining malignancies
Figure 2 shows the cumulative number of reported cases of malignancy. The most common malignancy was lung cancer, and a cumulative number of 150 cases was observed. Liver cancer was the most common malignancy until 2009; however, its incidence has decreased since then. Conversely, the incidence of lung cancer increased to 11 cases in 2010, and lung cancer was ranked first. Although the incidence of lung cancer has subsequently decreased, lung cancer has remained the most common malignancy in terms of cumulative incidence. Colorectal cancer is ranked second and gastric cancer third, followed by liver cancer. The malignancies that follow, in descending order, are anal, other hematologic, head and neck, other urological, and laryngopharyngeal tumors, and finally leukemia. In 2023 alone, 17 cases of colorectal cancer, 10 of anal tumors, 10 of gastric cancer, 6 of lung cancer, 4 of liver cancer, 3 of laryngopharyngeal cancer, and 2 of head and neck cancer were reported (Figure 3). Based on changes in the annual incidence of malignancies by infection route (Figure 4), homosexual transmission of HIV was the most commonly reported infection route. Regarding the characteristics of malignancies by infection route (Figure 5), remarkably, liver cancer cases accounted for approximately 50% of the cases of iatrogenic infection, mainly due to infection caused by the use of blood coagulation factor products in patients with hemophilia. The incidence of lung, colorectal, gastric, anal, and head and neck cancers was typically high among patients infected through homosexual transmission. The incidence of lung cancer was high regardless of the infection route. According to the distribution of peripheral cluster of differentiation (CD)4 cell counts at the onset of malignancies (Figure 6), more patients had lower counts of CD4 cells. However, the distribution gradient in patients with malignancies was smaller than that in patients with opportunistic infections (Figure 7). The distribution of patients who developed malignancies in 2023 showed a similar trend.
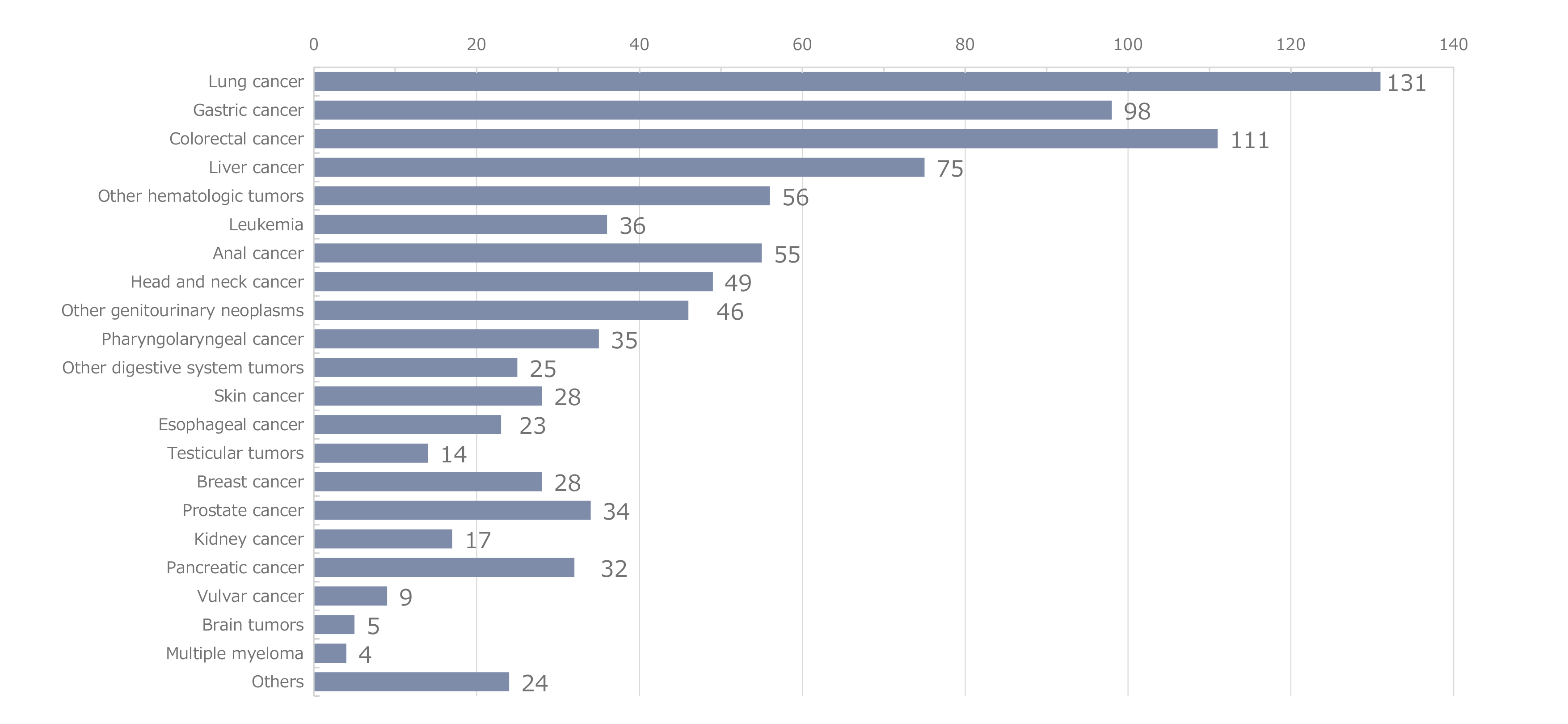
Figure 2. Number of reported cases of AIDS-defining malignancies by malignancy type
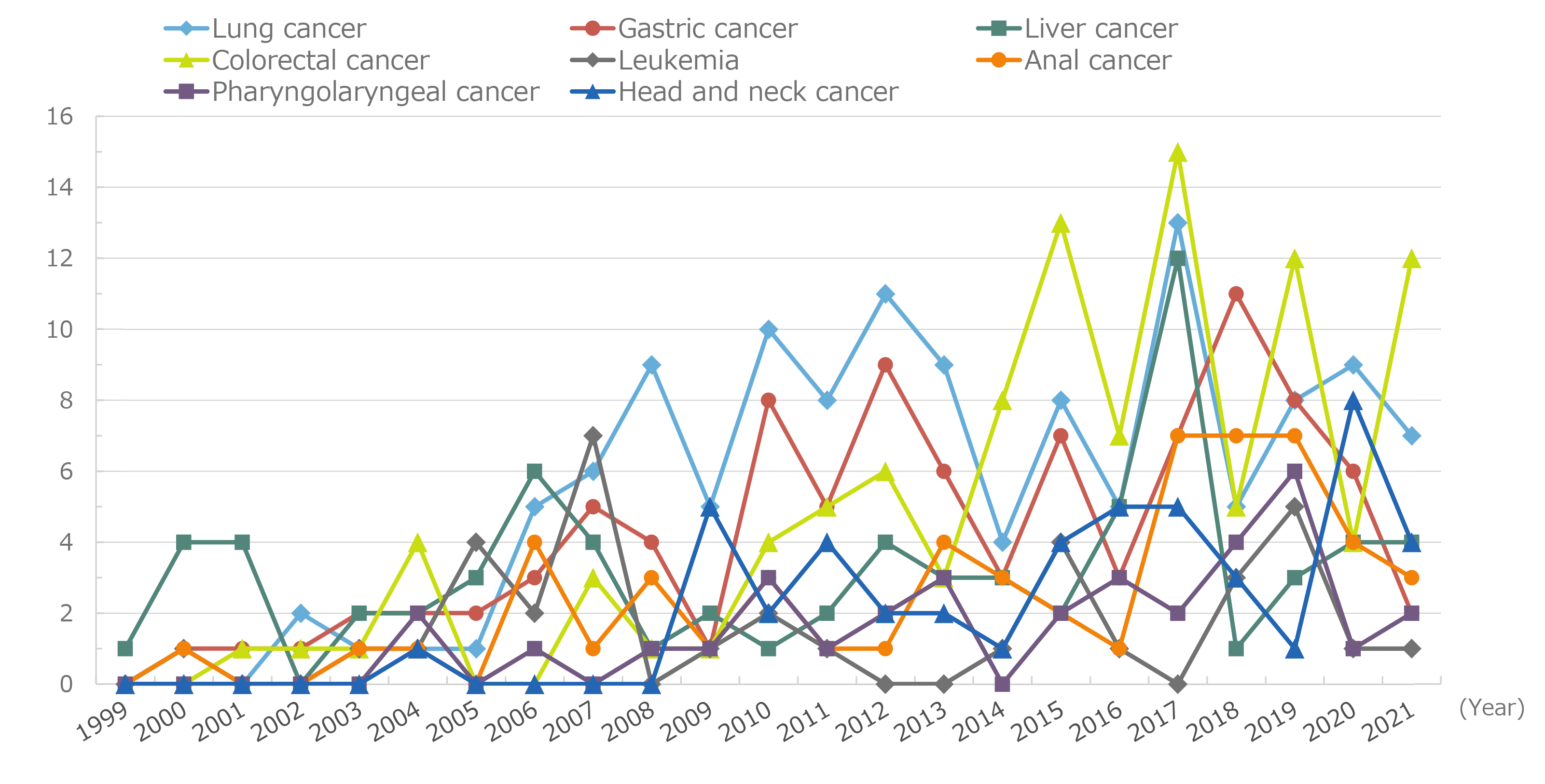
Figure 3. Annual changes in the incidence of major malignancies
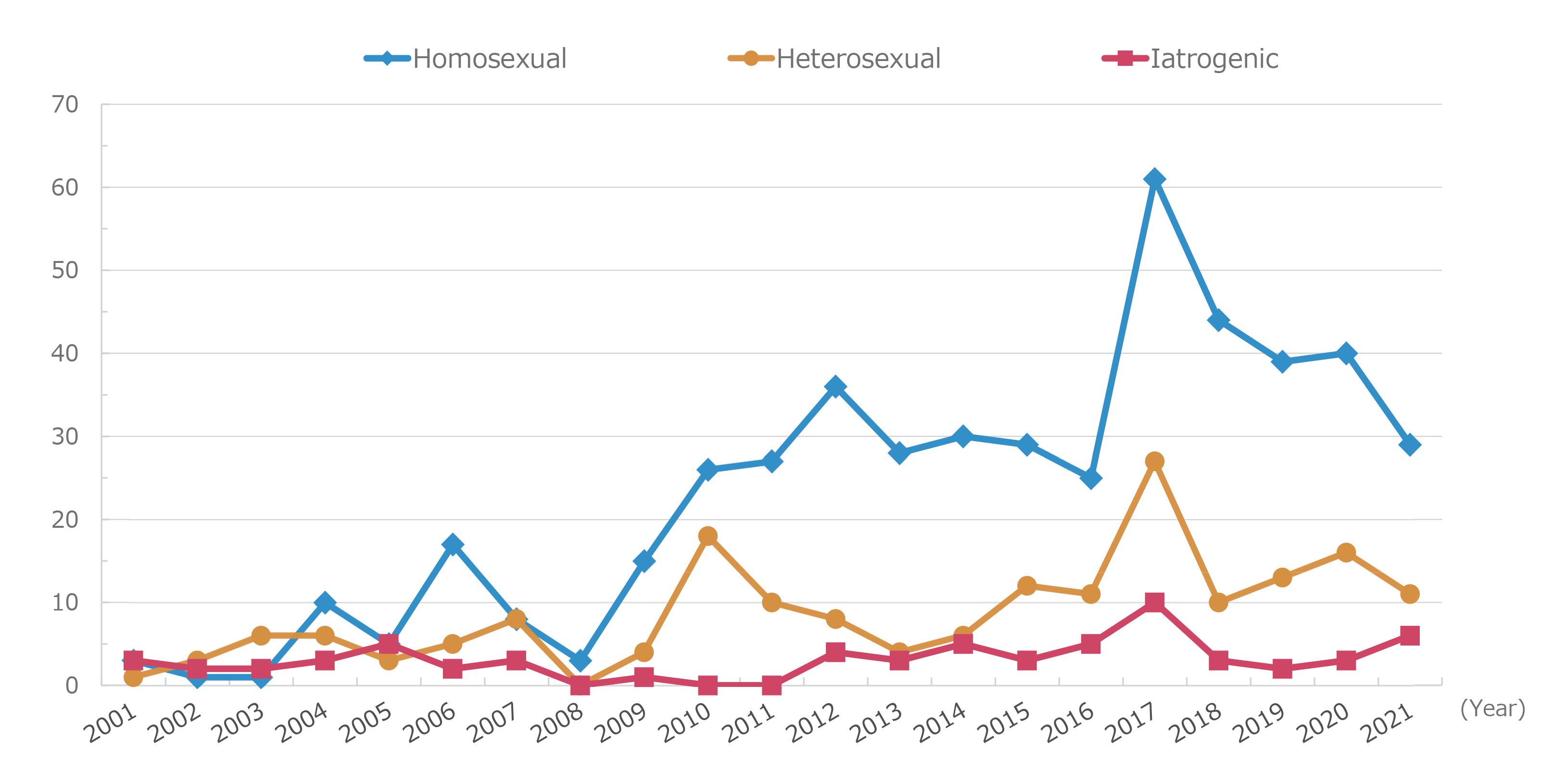
Figure 4. Annual incidence of malignancies by infection route
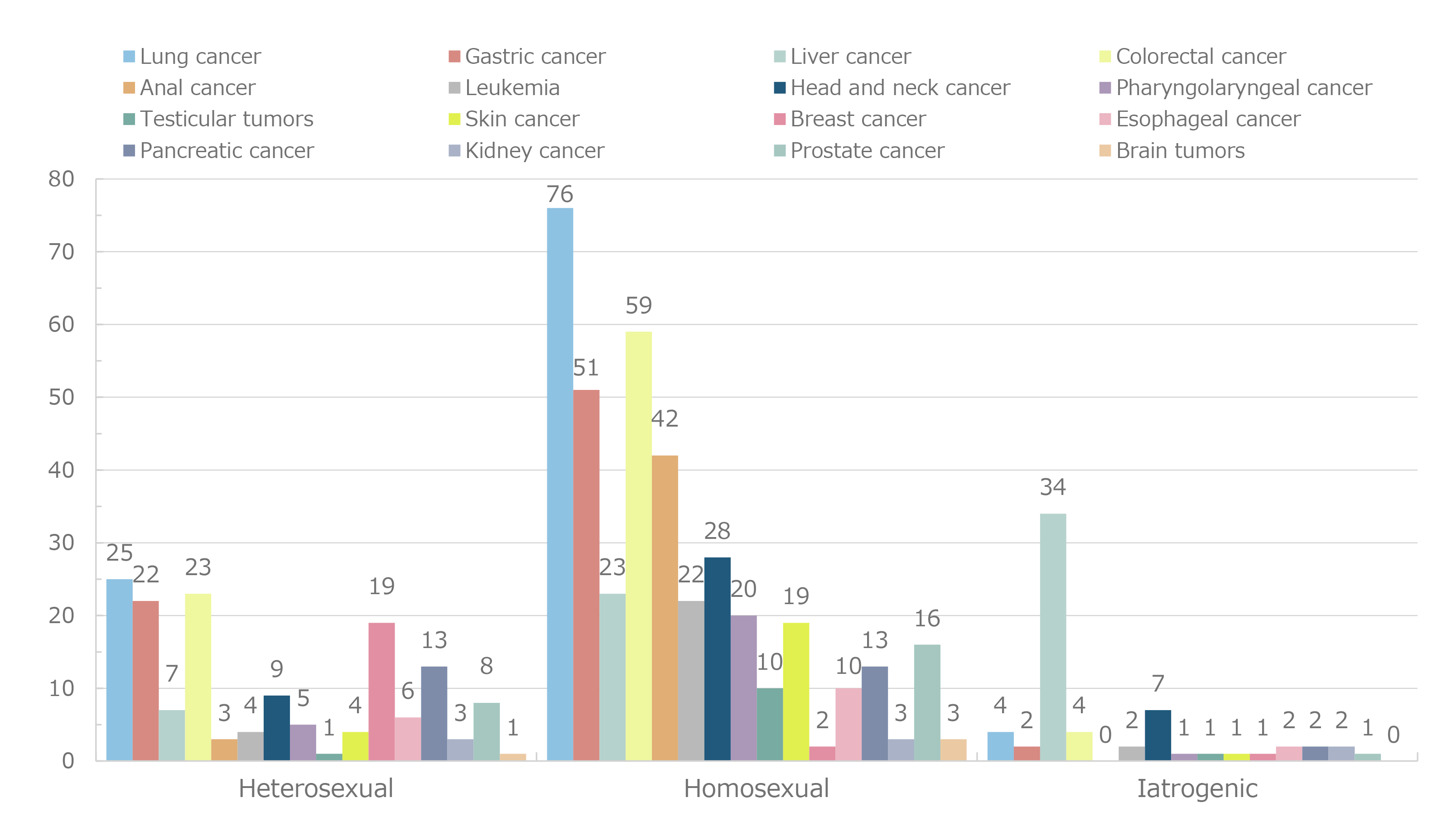
Figure 5. Incidence of malignancies by infection route
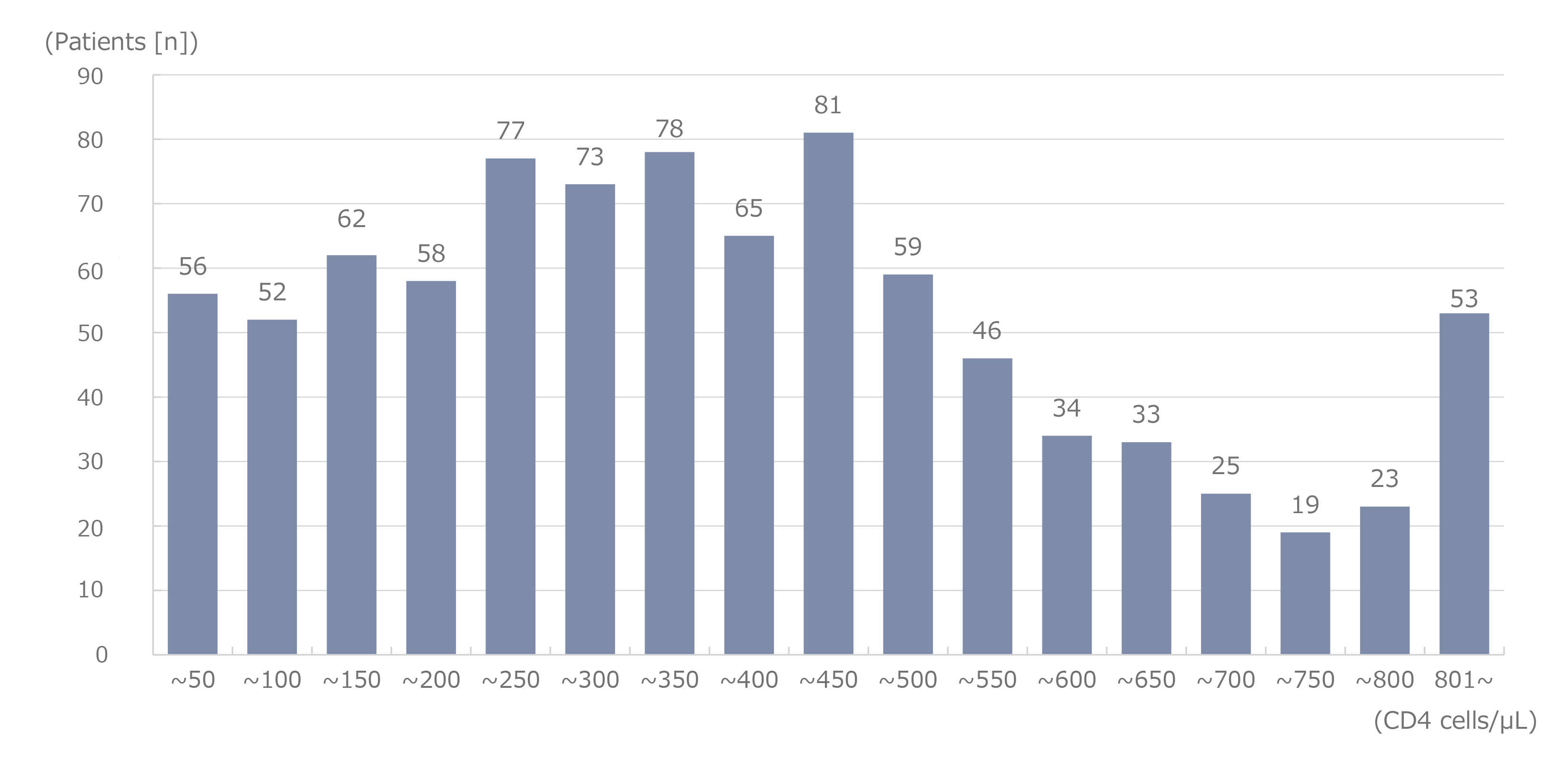
Figure 6. Distribution of CD4 cell counts at the onset of malignancies
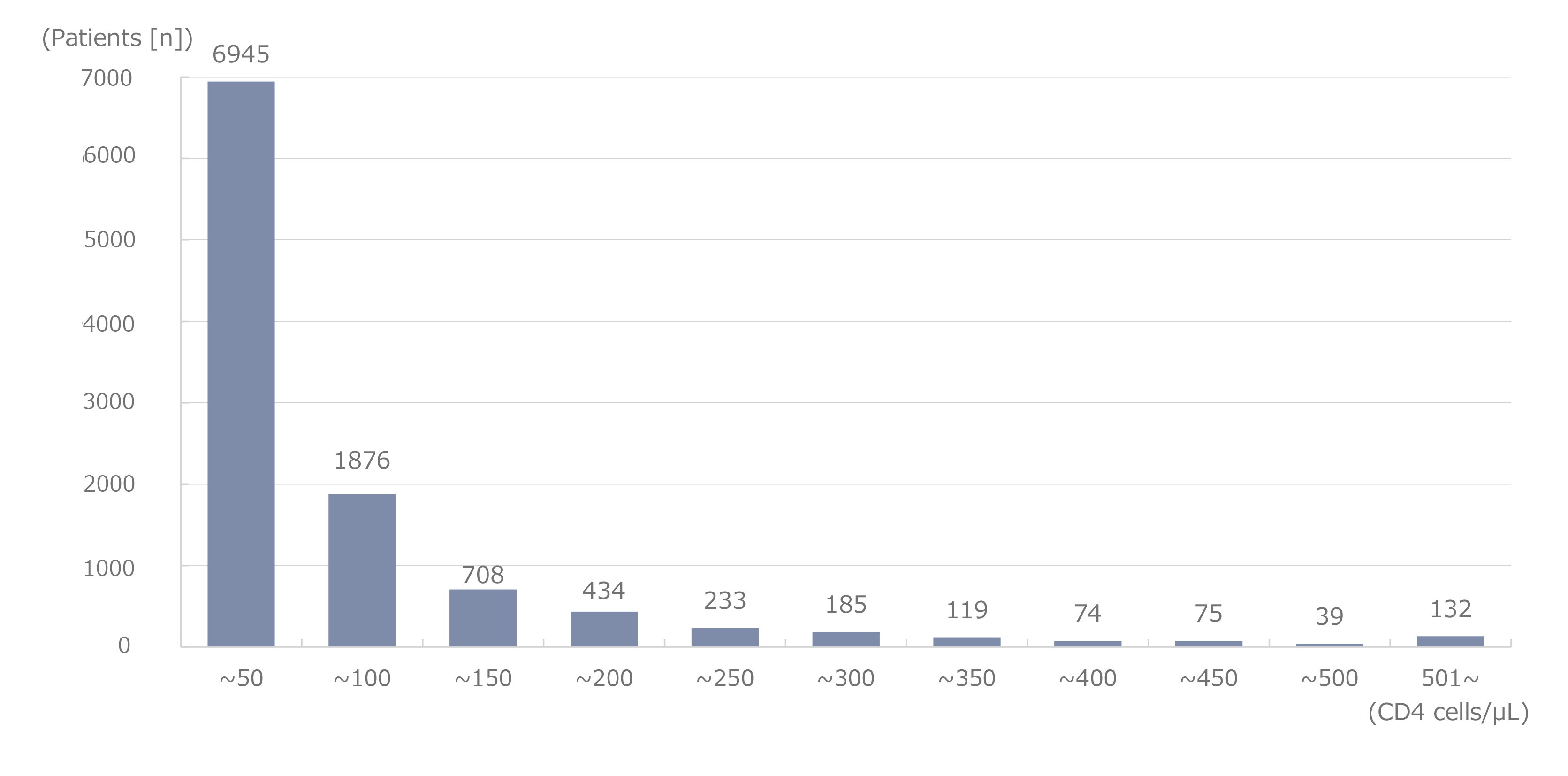
Figure 7. Distribution of CD4 cell counts at the time of opportunistic complications diagnosis
Figure 8 shows the distribution of CD4 cell counts by major malignancy type. CD4 cell counts varied widely regardless of the type of malignancy, and the distribution of CD4 cell counts was not polarized to any particular malignancy. The most common age at onset of malignancy (Figure 9) was 60–69 years. Older patients with HIV who developed malignancies were also included, as evidenced by the 2.0% incidence reported in the small population of patients with HIV who were in their 80s. Compared with the age at onset of opportunistic infections, which appears to be close to the age at which HIV infection is detected, the distribution of age at the onset of malignancy appeared to shift to older age. Based on the age distribution by HIV infection route (Figure 10), patients with iatrogenic infection tended to develop malignancies at younger ages than those infected through heterosexual or homosexual transmission. Based on age distribution by malignancy type (Figure 11), testicular tumors tended to develop at young ages. Regarding the time to onset of malignancy (Figure 12), more than 80% of all patients with HIV developed malignancies 1 year or more after being diagnosed with HIV infection. This contrasted with the time to onset of opportunistic infections, which occurred within 3 months (including simultaneous detection) in more than 80% of patients with HIV. This finding revealed that malignancies developed during a certain period of follow-up after diagnosis of HIV infection. Regarding the outcomes of those with HIV and malignancies (Figure 13), 63.1% of patients achieved complete and/or partial remission. Based on the mortality rate by malignancy type (Figure 14) the highest mortality rate was observed for pancreatic cancer—which is inherently associated with a poor prognosis—followed by leukemia, lung, esophageal, liver, and laryngopharyngeal cancers.
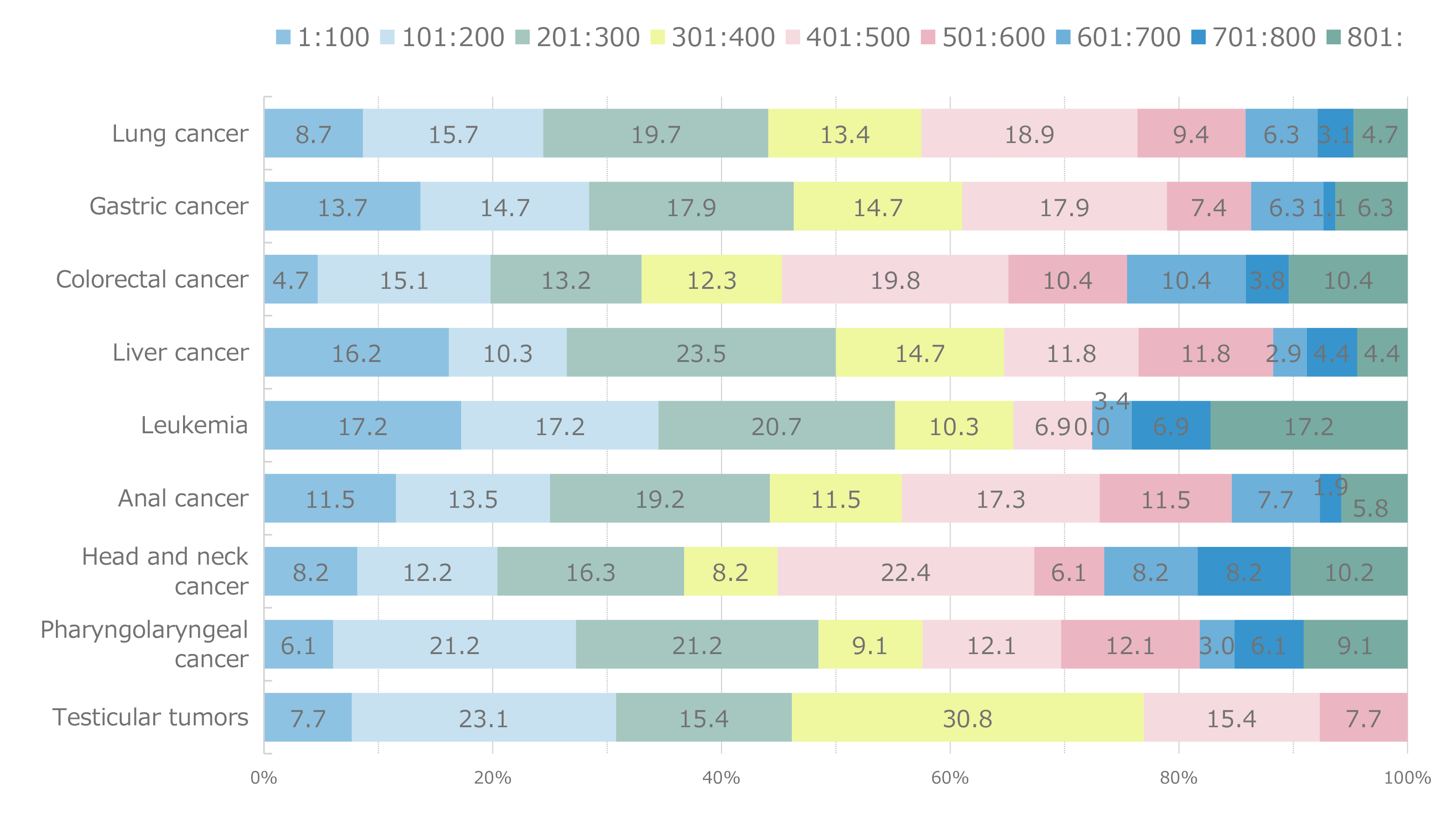
Figure 8. Distribution of CD4 cell counts at the onset of malignancies by malignancy type
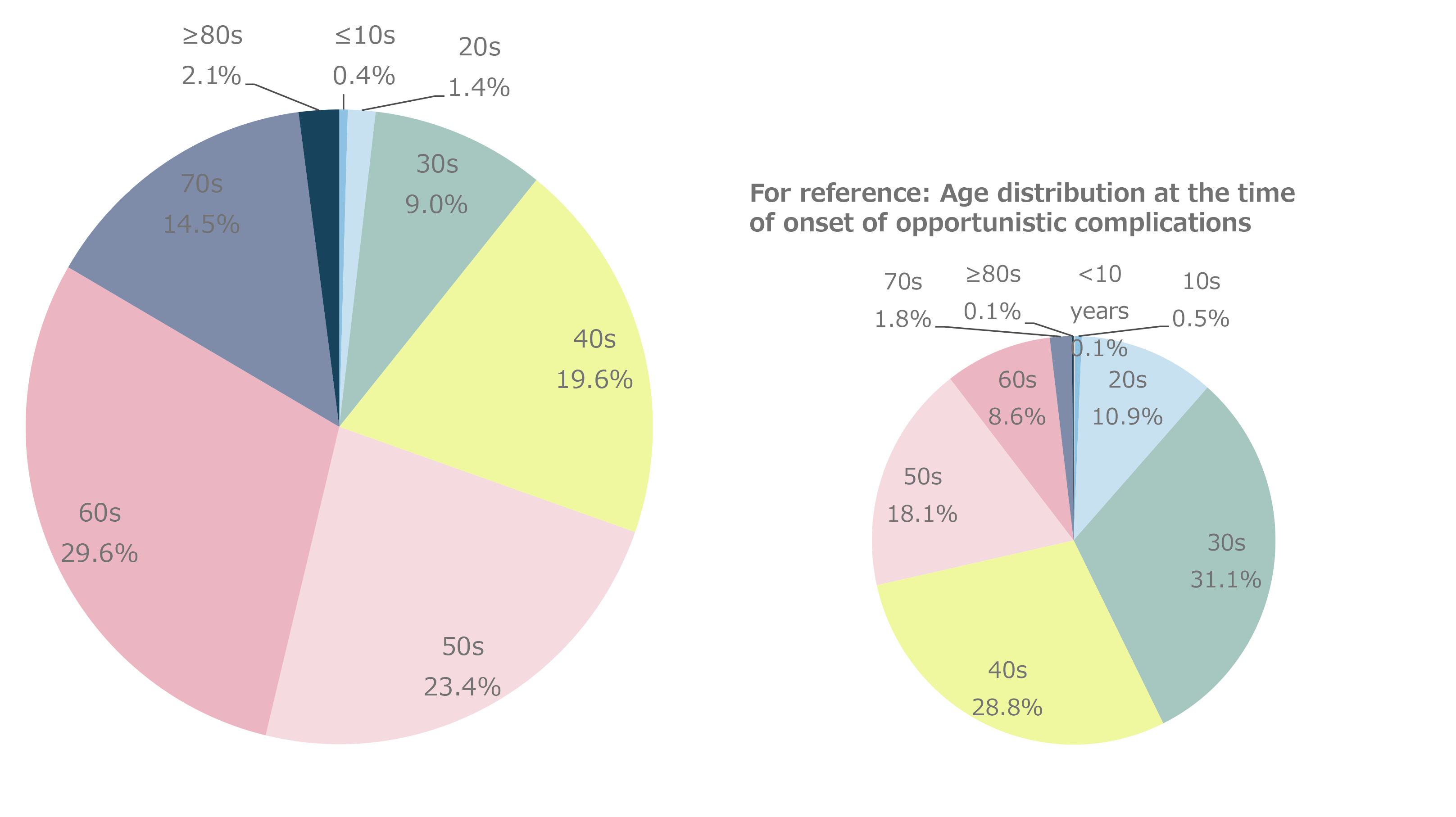
Figure 9. Age distribution at the onset of malignancies
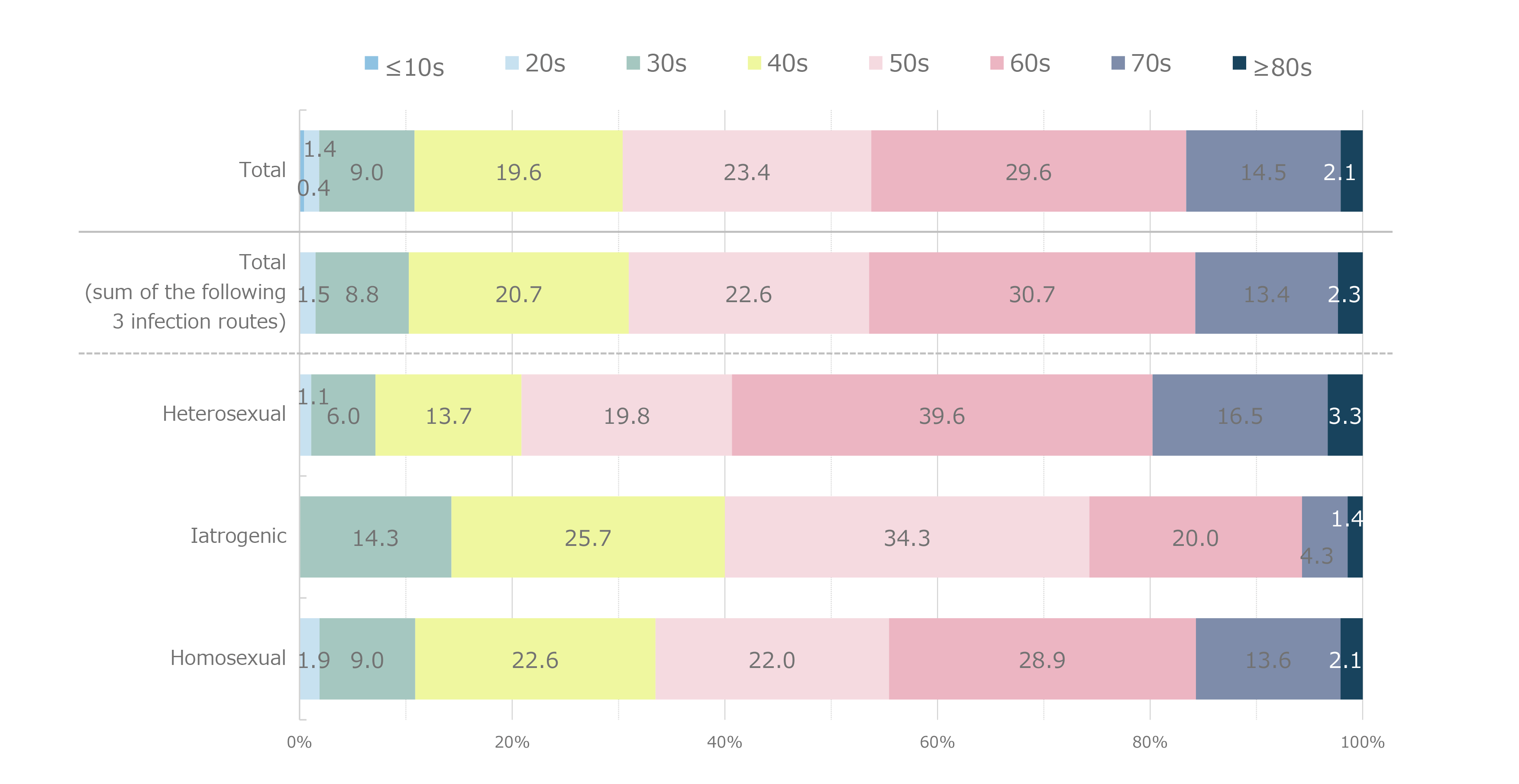
Figure 10. Age distribution at the onset of malignancies by infection route
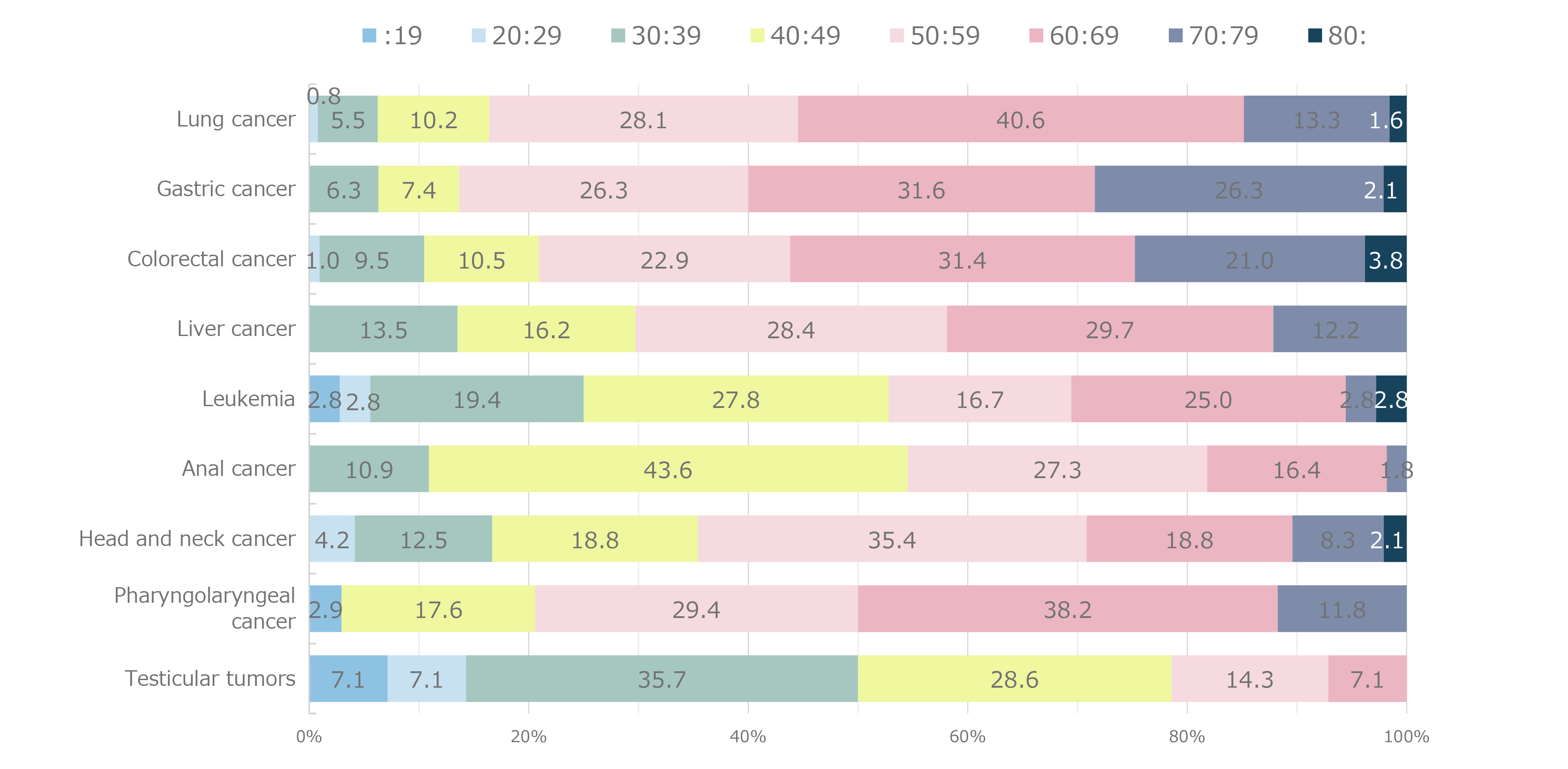
Figure 11. Age distribution at the onset of malignancies by malignancy type
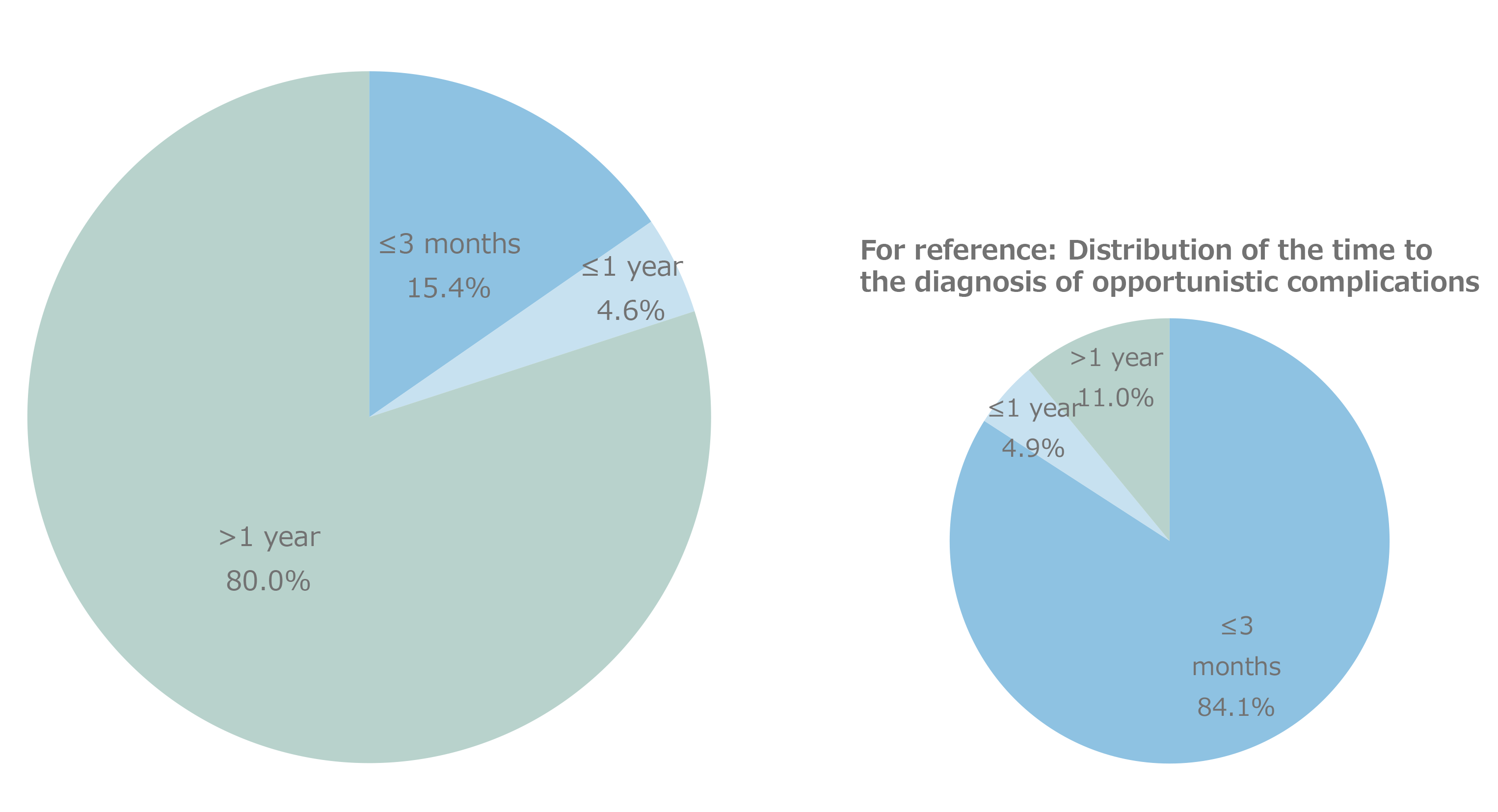
Figure 12. Time from the diagnosis of HIV infection to the onset of malignancies
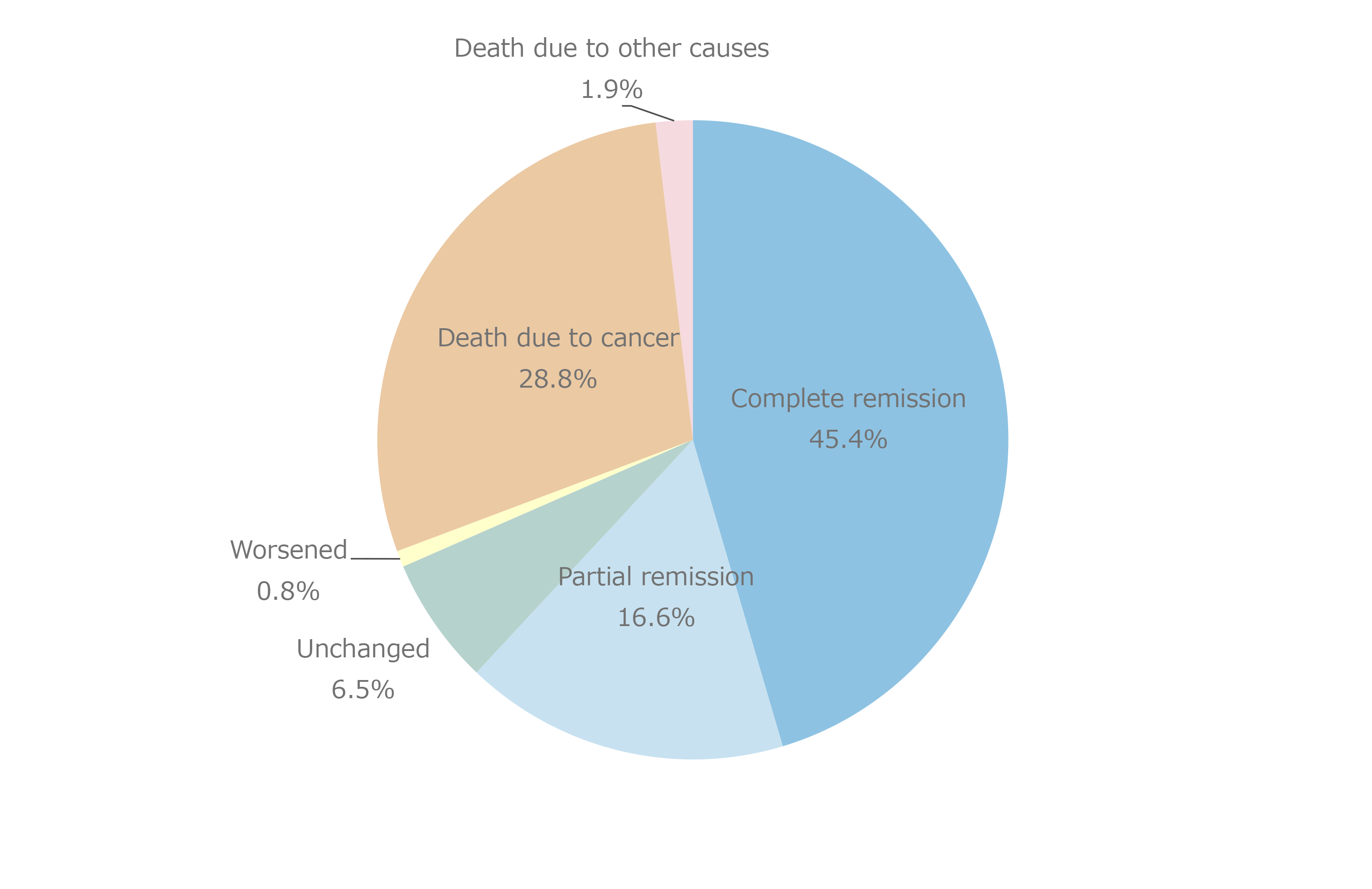
Figure 13. Outcomes of malignancies
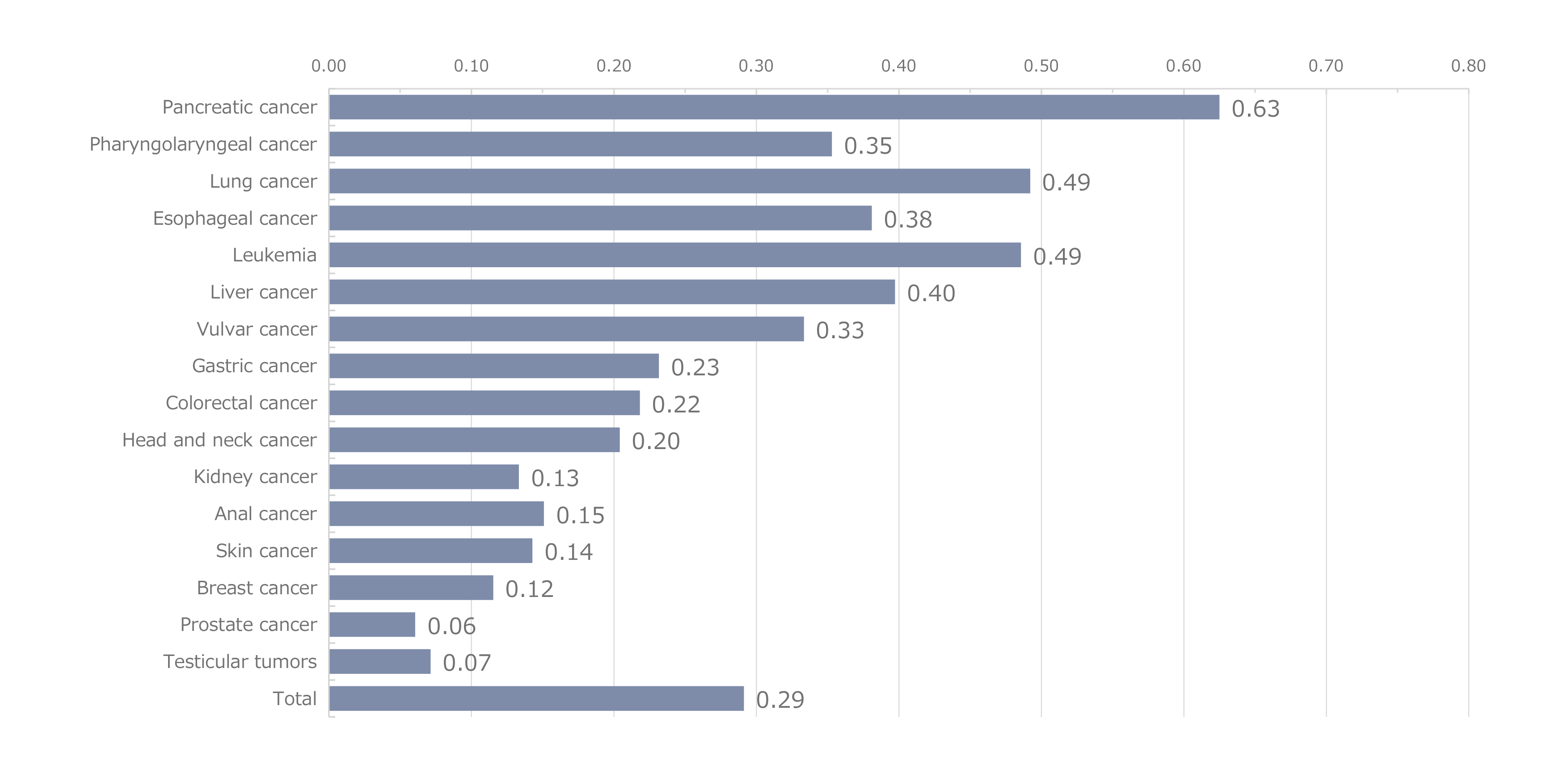
Figure 14. Mortality rates by malignancy type
D.Discussion
The introduction of antiretroviral therapy has enabled patients with HIV to remain in a stable condition for a long time, with the development of malignancies among these patients now becoming a concern. The present study was therefore initiated to address this concern. The findings of this study revealed that the incidence of non-AIDS–defining malignancies in patients with HIV was increasing each year in Japan. Previous studies have reported that the prevalence of malignancies in this patient population tends to be higher than that in the general Japanese population. In the present study, we found that when the age-adjusted prevalence in 2022 and 2023 was compared with that of a model population in 1985, the prevalence of malignancies in patients with HIV was 1.24 times higher than that in the general Japanese population. Given that some AIDS-defining malignancies—namely, malignant lymphoma, cervical cancer, and Kaposi’s sarcoma—were excluded from the aggregated data in the present study, the incidences of malignancies may be even higher. However, because the effects of HIV infection become evident sometime after infection with HIV, monitoring long-term changes appears necessary. The distribution of malignancies observed in patients with HIV was clearly different from that in the general population in Japan. Lung cancer, liver cancer, leukemia, head and neck cancer, laryngopharyngeal tumors, anal cancer, and testicular tumors were characteristically common in patients with HIV. Liver cancer has been suggested to be affected by concomitant infection with the hepatitis C and B viruses, and anal and other cancers have been suggested to be associated with infection with the human papillomavirus. Recent data indicate an association between lung cancer and viral infection. Particularly in Japan, the prevalence of leukemia is high. All subtypes of leukemia, namely, the myeloid, lymphatic, acute, and chronic subtypes, have been observed, and no characteristic differences exist among them. The annual incidence of eight major malignancies was evaluated and a sharp increase in the incidence of lung cancer was observed; this increase has been noticeable for the past few years. Despite the lack of definitive data, patients with HIV are highly likely to be predisposed to developing lung cancer and therefore susceptible to the effects of risk factors such as smoking. Thus, promoting smoking cessation in this patient population may be an important topic in the future. Furthermore, the incidence of colorectal cancer is increasing, and monitoring the future trends for this disease seems important. Liver cancer is presumed to be caused by coinfection with the hepatitis C virus that is transmitted through blood products. Although liver cancer was the most common malignancy until 2009, its incidence has since decreased. Therefore, monitoring the future trends in the incidence of liver cancer may also be necessary. Based on the distribution of CD4 cell counts at the onset of malignancies, the incidence of malignancies was higher in patients with a lower CD4 cell count. However, the distribution gradient was small, and the onset of malignancies was not as strongly associated with CD4 cell counts as with the onset of opportunistic infections. Malignancies mainly developed in patients aged 40 or older and were mostly detected after patients with HIV had been treated for 1 year or more. Even if the treatment administered for HIV infection leads to improved CD4 cell counts, the risk of developing malignancies will not be greatly reduced. Furthermore, because patients with HIV are treated for an extended period, they are likely to develop malignancies. Treatment of HIV infection includes achieving control through the administration of antiretroviral therapy and monitoring of metabolic complications: In future, to detect malignancies early, patients with HIV might need to undergo regular screening more frequently than individuals in the general middle-aged and older population who undergo outpatient screening.
E.Conclusion
We have investigated and characterized the incidence of malignancies in patients with HIV. In addition to the incidence of lung cancer, which was originally high, the incidence of colorectal cancer has rapidly increased recently. The factors leading to this increase need to be analyzed.